
Recurrent Pregnancy Loss by Dr. Sireesha Reddy

Recurrent Pregnancy Loss
Spontaneous pregnancy loss is a surprisingly common occurrence. Whereas approximately 15% of all clinically recognized pregnancies result in spontaneous loss, there are many more pregnancies that fail prior to being clinically recognized. Only 30% of all conceptions result in a live birth
Spontaneous pregnancy loss can be physically and emotionally taxing for couples, especially when faced with recurrent losses. Recurrent pregnancy loss (RPL), also referred to as recurrent miscarriage or habitual abortion, is historically defined as 3 consecutive pregnancy losses prior to 20 weeks from the last menstrual period. Based on the incidence of sporadic pregnancy loss, epidemiologic studies have revealed that 1% to 2% of women experience recurrent pregnancy loss.
CAUSES
Genetic Etiology
Approximately 2% to 4% of RPL is associated with a parental balanced structural chromosome rearrangement, most commonly balanced reciprocal or Robertsonian translocations.
Anatomical Abnormalities
Anatomic abnormalities account for 10% to 15% of cases of RPL and are generally thought to cause miscarriage by interrupting the vasculature of the lining of womb, prompting abnormal and inadequate placentation. Thus, those abnormalities that might interrupt the vascular supply of the lining of womb are thought to be potential causes of RPL. These include congenital uterine anomalies, intrauterine adhesions, and uterine fibroids or polyps.
The uterine septum is the congenital uterine anomaly most closely linked to RPL, with as much as a 76% risk of spontaneous pregnancy loss among affected patients. Other M?ªllerian anomalies, including unicornuate, didelphic, and bicornuate uteri have been associated with smaller increases in the risk for RPL.
The presence of intrauterine adhesions, sometimes associated with Asherman syndrome, may significantly impact placentation and result in early pregnancy loss. Intramural fibroids larger than 5 cm, as well as submucosal fibroids of any size, can cause RPL.
Infectious Causes
Certain infections, including Listeria monocytogenes, Toxoplasma gondii, rubella, herpes simplex virus (HSV), measles, cytomegalovirus, and coxsackieviruses, are known or suspected to play a role in sporadic spontaneous pregnancy loss. However, the role of infectious agents in recurrent loss is less clear. The most pertinent risk for RPL secondary to infection is chronic infection in an immunocompromised patient.
Endocrine Causes
Luteal phase defect (LPD), polycystic ovarian syndrome (PCOS), diabetes mellitus, thyroid disease, and hyper prolactinemia are among the endocrinologic disorders implicated in approximately 17% to 20% of RPL.
Poorly controlled type 1 diabetes mellitus is also associated with an increased risk of spontaneous abortion. Evaluation of endocrine disorders should include measurement of the thyroid-stimulating hormone (TSH) level. Other testing that might be indicated based on the patient's presentation include insulin resistance testing, ovarian reserve testing, serum prolactin in the presence of irregular menses, antithyroid antibody testing. Therapy with insulin-sensitizing agents for the treatment of RPL that occurs in the presence of PCOS has recently gained popularity.
Thrombotic Etiologies
Both inherited and combined inherited/acquired thrombophilias are common, with more than 15% of the white population carrying an inherited thrombophilic mutation.
The potential association between RPL and heritable thrombophilias is based on the theory that impaired placental development and function secondary to venous and/or arterial thrombosis could lead to miscarriage. Evidence that the transfer of nutrition from the maternal blood to the fetal tissues depends on uterine blood flow, and thus may be affected by thrombotic events occurring there, suggests a role for thrombophilias in pregnancy losses regardless of gestational age.
Appropriate therapy for heritable or acquired thrombophilias should be initiated once the disorder is diagnosed. Therapy is disorder specific and includes
(1) Supplemental folic acid for those patients with hyperhomocysteinemia
(2) Prophylactic anticoagulation in cases of isolated defects with no personal or family history of thrombotic complications
(3) Therapeutic anticoagulation in cases of combined thrombophilic defects.
Environmental Etiologies
Because of its propensity to result in feelings of responsibility and guilt, patients are often particularly concerned about the possibility that environmental exposures may have caused their pregnancy losses.
Three particular exposures-smoking, alcohol, and caffeine-have gained particular attention, and merit special consideration given their widespread use and modifiable nature. Although maternal alcoholism (or frequent consumption of intoxicating amounts of alcohol) is consistently associated with higher rates of spontaneous pregnancy loss, a connection with more moderate ingestion remains tenuous. Studies linking moderate alcohol intake with pregnancy loss have shown an increase in risk when more than 3 drinks per week are consumed during the first trimester or more than 5 drinks per week are consumed throughout pregnancy. It seems logical that cigarette smoking could increase the risk of spontaneous abortion based on the ingestion of nicotine, a strong vasoconstrictor that is known to reduce uterine and placental blood flow. However, the link between smoking and pregnancy loss remains controversial, as some, but not all, studies have found an association. Although still not undisputed, there appears some evidence that caffeine, even in amounts as low as 3 to 5 cups of coffee per day, may increase the risk of spontaneous pregnancy loss with a dose-dependent response. The association of caffeine, alcohol, and nicotine intake with recurrent pregnancy loss is even weaker than their associations with sporadic loss.
Prognosis
Although the diagnosis of RPL can be quite devastating, it can be helpful for the physician and patient to keep in mind the relatively high likelihood that the next pregnancy will be successful. A particular individual's prognosis will depend on both the underlying cause for pregnancy losses and the number of prior losses. Correction of endocrine disorders, APA, and anatomic anomalies enjoy the highest success rates, approximately 60% to 90%. Patients with a cytogenetic basis for loss experience a wide range of success (20% 80%) that depends on the type of abnormality present. Overall, the prognosis for RPL is encouraging. Even with the diagnosis of RPL and as many as 4 to 5 prior losses, a patient is more likely to carry her next pregnancy to term than to have another loss.
By
Dr. Sireesha Reddy | Know your doctor
Related Blogs

Understanding Gestational Diabetes: Insights from Dr Shruthi Kalagara
Read More
Urinary Tract Infection (UTI) in Pregnancy
Read More
Early Pregnancy Care for New Pregnant Women: Expert Advice | Motherhood Hospitals
Read More
Body Positivity Tips Post C Section (Cesarean Delivery)
Read More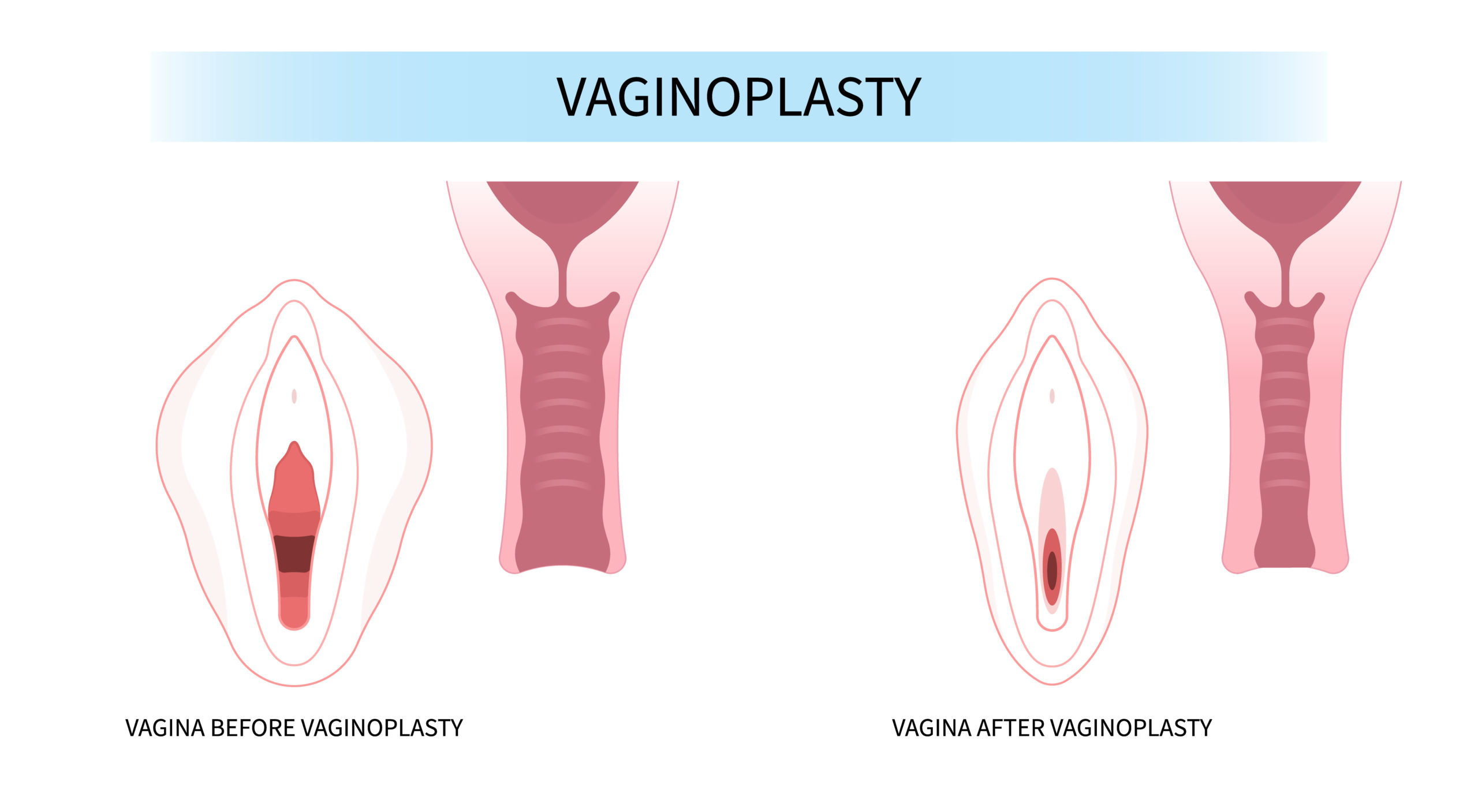
Vaginoplasty: Procedure, Cost, Risks & Benefits, Recovery
Read More
The Digital Dilemma: Exploring the Medical Implications of Technology on Child Development
Read More
How To Relieve Menstrual Cramps? - 8 Simple Tips
Read More
Benefits of Consuming Folic Acid Tablets For Pregnancy/During Pregnancy
Read More
Navigating Radiology: Ensuring Safe Imaging During Pregnancy
Read More
Navigating Radiological Tests During Pregnancy: Ensuring Safety for Mother and Child
Read MoreRequest A Call Back
Leave a Comment:
View Comments
Previous
Next
HELLO,
Stay update don our latest packages, offer, news, new launches, and more. Enter your email to subscribe to our news letter


 Toll Free Number
Toll Free Number







No comment yet, add your voice below!