
Gestational Diabetes

It is a state of increased sugar level which generally normalizes after childbirth.
This occurs due to increased sugar level during pregnancy which is due to decreased insulin production or insulin resistance.
Incidence 10% of the population is affected by GDM and it is increasing due to advanced maternal age and sedentary lifestyle.
Why does it occur- During pregnancy, an organ called placenta is formed which provides food and oxygen to the baby from the mother. This also produces certain hormones which prevent the action of Insulin on sugar. This increases the sugar level in pregnant patient's blood. Our pancreas produces insulin, but as the sugar during pregnancy is already high the amount of insulin produced is not enough to metabolize sugar resulting in increased sugar level.
Risk factors for GDM
- PCOS-Polycystic ovarian disease
- Obese patient with BMI more than 30
- Previous history of having diabetes during pregnancy.
- History of diabetes in a family
- Having the previous baby of more than 4 kg
- History of sudden still birth or IUFD.
- An elderly primi
- Ethnic-origin east Asian
- Increased thirst
- Increased urination
- Weakness
- Increased appetite
- Abdominal circumference is more than gestational age in growth scan at 28 weeks
- Amniotic fluid is more than 20.
- Breathing difficulty due to increased girth
- Repeated vaginal infection
- High blood pressure
- Sometimes retinal detachment due to small vessel damage
- Macrosomia or big baby
- Difficult shoulder delivery during birth
- Inside uterus death of a baby (IUFD)
- Post-delivery hypoglycemia of baby management
- If GCT at 28 weeks more than 140 or above>
- Prolonged labor
- Shoulder dystocia (shoulder can get stuck)
- Perineal laceration
Related Blogs

Understanding Gestational Diabetes: Insights from Dr Shruthi Kalagara
Read More
Urinary Tract Infection (UTI) in Pregnancy
Read More
Early Pregnancy Care for New Pregnant Women: Expert Advice | Motherhood Hospitals
Read More
Body Positivity Tips Post C Section (Cesarean Delivery)
Read More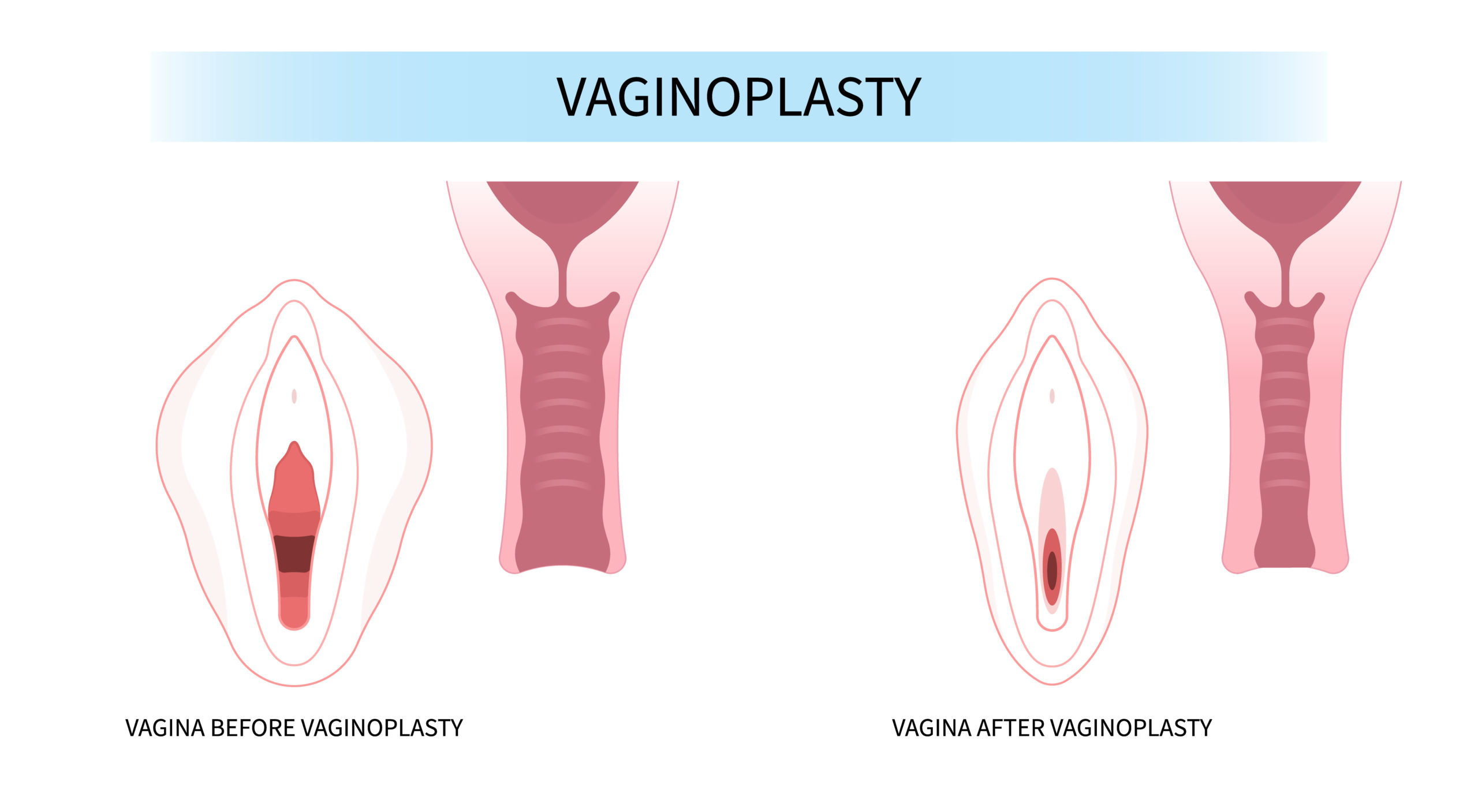
Vaginoplasty: Procedure, Cost, Risks & Benefits, Recovery
Read More
The Digital Dilemma: Exploring the Medical Implications of Technology on Child Development
Read More
How To Relieve Menstrual Cramps? - 8 Simple Tips
Read More
Benefits of Consuming Folic Acid Tablets For Pregnancy/During Pregnancy
Read More
Navigating Radiology: Ensuring Safe Imaging During Pregnancy
Read More
Navigating Radiological Tests During Pregnancy: Ensuring Safety for Mother and Child
Read MoreRequest A Call Back
Leave a Comment:
View Comments
Previous
Next
HELLO,
Stay update don our latest packages, offer, news, new launches, and more. Enter your email to subscribe to our news letter


 Toll Free Number
Toll Free Number







No comment yet, add your voice below!