
Baby Care and breastfeeding when you have COVID-19


Breastfeeding in a pandemic: An overview:
COVID-19 is disrupting various routines worldwide. Every front of human life is under dispute and disharmony. The pandemic warrants quick actions under clinical observations. When a breakthrough becomes available, it may require subsequent guidelines to establish proper care. Breastfeeding is essential to optimize neonatal health. The health and growth benefits of breastmilk are undisputed and demonstrated. To establish secure breastfeeding in a pandemic like COVID-19, we should thoroughly understand the effects of the pandemic on maternal and neonatal health.
First of all, we should understand how the clinical characteristics of COVID-19 apply to breastfeeding. We should even understand the protective properties of breastfeeding. The tenets of neonatal healthcare may even include the importance of skin-to-skin care. The evidence available till today suggests that the risk of transmission of COVID-19 via breastmilk is very low. Breastfeeding is known for its irreplaceable health benefits both for the mother and the baby. Infection control strategies should be in place with stiff adherence to them.
How to uphold care and caution while breastfeeding during the pandemics like COVID-19?
World Health Organization (WHO) rules that mothers with COVID-19 or suspected to carry the virus may opt to breastfeed their babies provided they follow every safety protocol. Breastfeeding is likened to promote anti-inflammatory responses along with antimicrobial properties and healthy immune responses. The components in breastmilk may also help prevent the incidence of respiratory tract infections. Breastmilk is loaded with an irreplaceable nutritional value contributing to the healthy growth of infants.
Even breastfeeding from women with confirmed or suspected COVID-19 infection can benefit the infants. Breastmilk constitutes a primordial form of health and development in infants. Breastfeeding establishes itself as the ideal food for kids during the first 6 months. With an irreplaceable nutritive value, it betters the immune response of kids strengthening the defense mechanisms against common and opportunistic infections. Regular and frequent breastfeeding also associates itself with a decrease in neonatal morbidity and mortality.
How does the risk of COVID-19 endanger pregnancy and breastfeeding?
Current evidence is unclear about the vertical transmission of COVID-19 from the mother to her foetus through the placenta in pregnancy. Studies found no traces of the virus in amniotic fluid, placental tissue or umbilical cord blood. As stated above, the traces of novel coronavirus weren't found in the breastmilk. Precautions are necessary to ensure a low risk of COVID-19 in babies and mothers who are breastfeeding. Mother-infant proximity is a healthy practice even amid the pandemics provided every safety protocol is in place. Healthcare professionals may extend their support to mothers who are unable to breastfeed in the wake of serious complications of COVID-19.
The women who are unable to breastfeed their baby may avail themselves of alternative methods. They may seek help from certified donor milk bank services or other centres dedicated to uplifting breastmilk supply. WHO recommends exclusive breastfeeding for the babies during the first 6 months of life. Even after including solid food in the diet of a child, mothers may continue breastfeeding their kids for 6 additional months. They may uphold this practice till the child reaches the age of 2. Mothers with COVID-19 must realize the importance of breastfeeding and opt for the same under stiff obstetric supervision.
Why do people worry about the effects of COVID-19 on pregnancy and breastfeeding women?
Pregnant women aren't more likely to fall prey to the COVID-19 infection than the nonpregnant counterparts. However, pregnancy itself involves many physiological changes including changes in the immune system and its response to the virulent microorganisms including COVID-19. Therefore, the incidence of COVID-19 in pregnancy may often relate to more severe symptoms of COVID-19. The COVID-19 pneumonia cases reported to date include mild to moderate symptoms and carry fair rates of recovery.
Pregnant women with other conditions such as hypertension, diabetes or high body mass index may develop complications following exposure to COVID-19. The pandemic itself may raise the risk of prenatal depression and anxiety in women. It may be important to extend proper obstetric care to pregnant and breastfeeding women.
How to regularize breastfeeding and postnatal care in the pandemics like COVID-19?
More studies are needed to confirm whether the high-risk newborn babies are at a raised risk of complications or not. Infection of COVID-19 following any contact with virulent respiratory secretion may be a cause of concern. The healthcare staff and facilities may consider temporary separation in the event of maternal COVID-19 infection.
Please follow the guidelines below if you find that temporary separation is mandatory:
- The healthcare team should assess the risks and benefits of temporary separation and communicate the same to the mother.
- The infants should be availed of a separate isolation room.
- In the event of the clinical obligations for colocation (rooming-in), of the baby and his/her sick mother in the same facility, facilities should consider every important aspect to prevent the transmission of COVID-19 from mother to child.
- The staff at the healthcare facility might consider using physical barriers to maintain safe distances between the mother and her child.?
- If there's nobody to look after the new-born baby except the mother (COVID-19 infected or suspected) herself, the mother should maintain hygiene and practice hand sanitization under obstetric guidance. These standards should continue as long as the mother is under observation for the possibility of vertical transmission.
Breastfeeding:
- Mothers willing to breastfeed their babies even under temporary separation should consider expressing their milk.
- Expressing milk offers various health benefits both to the mother and her baby including establishment and maintenance of the proper milk supply.
- Mothers can use dedicated breast pumps for seamless milk extraction.
- Mothers should accustom themselves to safety protocols and hand hygiene as they start expressing breastmilk.
- After each session of milk extraction, every part of the pump should be sanitized and disinfected as directed by the manufacturer/medical official.
- Healthcare teams should include a healthy caregiver to ensure proper distribution and consumption of the expressed breastmilk.
- The mother and baby in colocation should be under proper clinical observation.
- The mother willing to feed the baby at the breast should always wear the facemask alongside the appropriate standards of hand hygiene before and after each feed.
Related Blogs

The Digital Dilemma: Exploring the Medical Implications of Technology on Child Development
Read More
How To Relieve Menstrual Cramps? - 8 Simple Tips
Read More
Benefits of Consuming Folic Acid Tablets For Pregnancy/During Pregnancy
Read More
Navigating Radiology: Ensuring Safe Imaging During Pregnancy
Read More
Navigating Radiological Tests During Pregnancy: Ensuring Safety for Mother and Child
Read More
Decoding the Wonders of Pregnancy: When and Why Ultrasound Scans Take Center Stage
Read More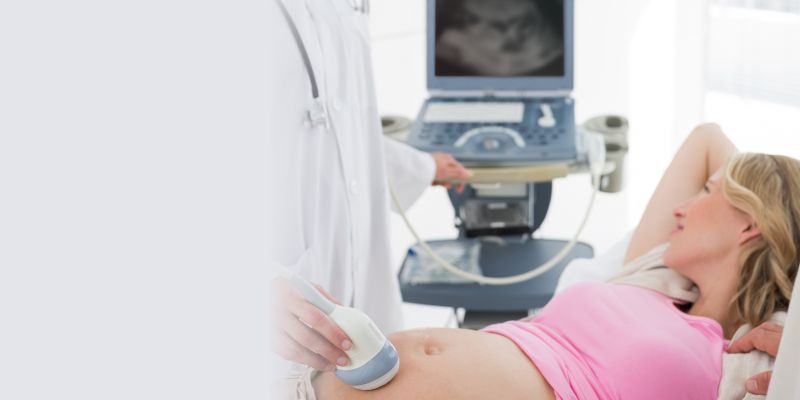
Decoding the Wonders of Doppler Ultrasound in Pregnancy: A Radiologist's Perspective
Read More
Understanding Cervical Cancer: The Crucial Role of Early Preventive Health Checks
Read More
I Am Very Fortunate: Embracing the Gift of Parenthood with Motherhood Fertility and IVF
Read More
Navigating Infertility - A Roadmap to Hope and Parenthood
Read MoreLeave a Comment:
View Comments
Previous
Next
HELLO,
Stay update don our latest packages, offer, news, new launches, and more. Enter your email to subscribe to our news letter


 Toll Free Number
Toll Free Number







No comment yet, add your voice below!